If you have gone to the doctors recently they may have talked to you about your body mass index or BMI. BMI can easily be calculated with only a basic scale and tape measure, all you do is take your weight and divide it by your height. Here is a link to a simple calculator you can use if you are curious what your BMI is.
BMI is a common measurement used by medical professionals to determine whether someone is underweight, normal weight, overweight or obese. Below is a table that illustrates the breakdown of the different classifications.

But why is BMI even used?
In general BMI is used to assess how much body fat you have. The general assumption is the higher your BMI the more body fat you have.
What is so bad about body fat?
The amount of body fat you have or do not have also has a strong CORRELATION (remember correlation is not the same as fact) to your health. In general, and we will go into this in further detail later on in this post, the higher your body fat the more likely you are to have poor health.
If we assume BMI is a proxy for how much body fat you have then we can also conclude the higher your BMI the poorer your health.
It turns out though that it is very easy to poke holes in many of the long held beliefs and assumptions around BMI.
While BMI is associated with the amount of body fat you have, it is calculated using your weight, which is not a direct measure of your body fat. Instead your weight is made up of everything in your body which includes body fat, but also the food you just ate, the water you drank, the bone in your body, and your muscle mass. While it’s incredibly hard to change your bone, or eat enough food or drink enough water to drastically affect your BMI, it is possible (over the course of several years and with A LOT of hard work) to gain enough muscle to make a meaningful difference in your BMI. Many well muscled people can fall in the overweight and obese categories purely because of the amount of muscle they have on their body.
In addition, there are people who have a lot of body fat, to the point that most people would consider unhealthy, yet have no indications of poor health. These people are often referred to as “metabolically healthy obese”.
Another criticism of BMI is that it also fails to differentiate between the different types of fat on our body. There are 3 types of fat found in our body, subcutaneous fat is the fat that sits right below the skin, it’s the fat that you feel when you pinch your belly or arm or thighs. While subcutaneous fat might be aesthetically unappealing to some, it’s actually the least dangerous from a health perspective.
The much more dangerous type of fat is the fat found around your organs, often called visceral fat. When we start storing fat around our organs it’s a sign that we have exceeded our fat threshold, our body has run out of places to put fat and as a last resort has placed it around our organs. The best example of this is when fat gets stored around your liver, this is often referred to as fatty liver. It is very common among alcoholics, but also can happen without drinking alcohol due to over consuming calories.
Just like we see people who have plenty of body fat and are overweight and obese but are perfectly healthy, we can also find people who appear to have low levels of body fat but have high amounts of visceral fat. In other words a doctor could see someone has a normal BMI but has high levels of visceral fat and would never know that their health is compromised just by using BMI.
The association between body fat and BMI was studied in white European men so it can be inaccurate in people of other ethnicities. This means the same BMI in a white male may have more or less risk associated with it in someone of a different ethnicity.
Finally BMI can also introduce some level of bias in the healthcare system, where those with higher BMI often receive poor levels of care (Weight Bias and Health Care Utilization: A Scoping Review, 2019).
Given all this you are probably thinking BMI is useless and to some degree, harmful. I can’t blame you, it is no doubt a flawed metric.
That said, we do have some data that shows BMI can be useful.
One study done on participants of the Framingham Heart Study showed a strong correlation between maximal BMI and mortality over the course of the 24 years. (Association of Obesity With Mortality Over 24 Years of Weight History: Findings From the Framingham Heart Study, 2018).
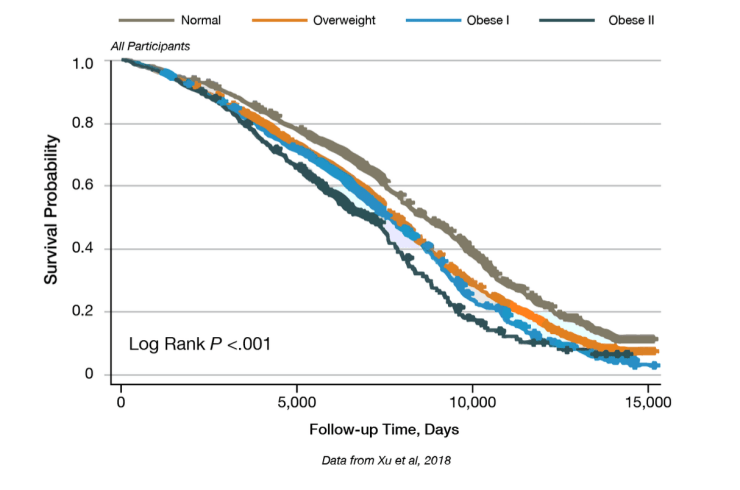
As you can see if you maintained a normal BMI over the course of the 24 years you had the highest survival probability across the entire duration. Next was overweight followed closely by class 1 obesity and finally class 2 obesity.
One interesting thing to call out about this data is that researchers used maximal BMI reached over the duration of the study. This is interesting when we look at this second figure from the study.

It shows that the negative effects of obesity probably don’t reverse all together even if you lose weight. Don’t get me wrong, I am not suggesting that losing the weight isn’t better than maintaining the weight, it just doesn’t undo the harm.
I will also state upfront that since this data is coming from the Framingham Heart Study the population was predominantly white individuals of European descent, so again we have to keep in mind that this may not apply to other ethnicities (Kannel, 2015).
Another study looked at the prevalence of metabolic syndrome and BMI. Someone is said to have metabolic syndrome if they have 3 or more of the following symptoms:
- Elevated triglycerides (≥150 mg/dL).
- Low HDL-C (<40 mg/dL for males or <50 mg/dL for females).
- Elevated fasting plasma glucose (≥110 mg/dL) or a diabetes diagnosis.
- High blood pressure (systolic blood pressure ≥ 130 mmHg or diastolic blood pressure ≥ 85 mmHg) or a hypertension diagnosis.
- Waist circumference
- US: >102 cm for males or >88 cm for females
- International Diabetes Foundation: ≥94 cm for males or ≥80 cm for females (mostly caucasian individuals)
Researchers used data from just over 14,000 men and women from Tel Aviv. (They did not break out ethnicities in this paper.)
Here is what they found…
Only 7.5% of obese participants had none of the symptoms of metabolic syndrome. For those that had class 2 obesity or greater, that number dropped to 1%.

https://www.ncbi.nlm.nih.gov/pmc/articles/PMC10215588/
However the researchers also found that even those with a normal BMI 20% had at least one of the criteria for metabolic syndrome.
Researchers also found that age plays a role in risk of metabolic syndrome as well irrespective of BMI.
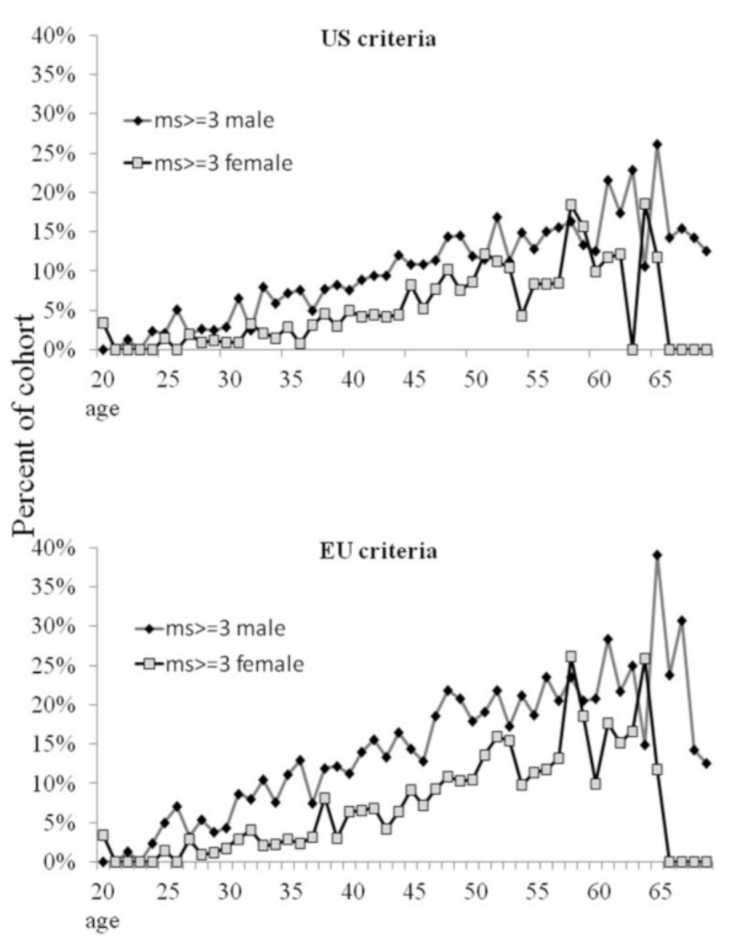
Keen observers looking at the graphs above will also notice that being a female appears to be more “protective” of metabolic syndrome than being male when just looking at age.
While some of the data from this paper certainly verify some of the criticisms of BMI it also provides some additional evidence that the higher your BMI the more likely you are to have metabolic syndrome.
Where does that leave us with BMI?
I am not a medical professional and I don’t measure peoples BMI, nor do I ask for it when speaking to clients, so take what I am about to say purely as my own opinion and not backed up by any personal experience.
I think this quote sums up my thoughts on BMI…
“Despite being a practical tool for evaluating obesity and predicting chronic disease and mortality in a large population, the use of BMI to identify excess fat at the individual level has reasonable specificity but poor sensitivity…” (de Carvalho, 2023)
What the authors of this paper are basically saying is when you look at BMI across a large number of people it can provide some useful information regarding the amount of body fat one carries. However if you drill down to the individual level it can be less useful.

If we look at this graph, there is a pretty strong correlation between body fat percentage measured via a DEXA scan (often considered the gold standard in body composition analysis) and BMI. However there are some dots on that graph, which represent an individual in the study, that stray far from the trend line. These represent individuals in which BMI does not correlate with the amount of body fat they are carrying.
In this image we see from the same dataset how many people actually had excess body fat despite having a normal BMI.

But we can also see how few people did not have excess body fat once you get into the overweight and obese BMI categories.
Let’s sum all this up by making this a bit more practical.
If I was in the overweight or obese BMI category AND my diet did not consist of whole foods AND I was not consistently exercising I would personally be a bit concerned about the status of my health.
Could I still be metabolically healthy in this case despite potentially having excess body fat?
Sure I could be, the chances are small, but there is still a chance.
However in my opinion even if you find you are still metabolically healthy in this case, that is just a point in time statement, it is not a done deal. Your chances of developing metabolic syndrome will go up, just by the mere fact that everyday you get older you are more at risk of developing metabolic syndrome. Carrying around excess body fat into old age with poor lifestyle habits is just asking for trouble in my opinion.
If this were me and I was classified as metabolically healthy obese I would consider myself lucky and start taking steps to improve my lifestyle.
If I had a BMI in the overweight or obese category and my diet was dialed and I was clearly a well muscled individual, I would not pay attention to it at all and rely on my blood work and annual physical to determine my health status.
If I had a normal BMI but did not exercise and did not have the best diet, I would not let my normal BMI be a free pass to not dig deeper into my health. There is a chance that I could be carrying excess body fat and still have some markers of poor metabolic health then I would be getting my blood work done and using my annual physical to make sure my health was OK.
Even if those came back fine I would still be thinking about adding in some exercise at the very least in order to make sure I can maintain the muscle I have as I age. (Age will eat away at your muscle mass and that can put you into the excess body fat category without you even gaining additional fat!)
If I had a normal BMI and had a decent diet and was exercising regularly I would be fairly certain my health is OK, but even here I would still personally confirm this with blood work at least once a year just to keep an eye on things.
I will also say that making changes to improve your health does not necessarily mean lowering your BMI if you fall into the overweight or obese category. There are many “weight neutral” lifestyle changes you can make to improve your health that have nothing to do with weight loss.
For example, improving your diet quality, getting more sleep, or meditation. These can have drastic impacts on your health even if your body fat levels stay the same. Hell, you could even gain weight by strength training and increase your BMI but make dramatic changes to your health by doing so. Bottom line is when I say I would “make changes” in the paragraphs above that does not necessarily mean you need to lower your BMI.
We also have the consideration of ethnicity when taking into consideration BMI. You should know that a majority of the data we have has been collected with caucasian and african americans (How Useful Is Body Mass Index for Comparison of Body Fatness Across Age, Sex, and Ethnic Groups?, n.d.). There have been other studies showing that BMI is less accurate in other ethnicities (Correlation Between Epicardial Adipose Tissue and Body Mass Index in New Zealand Ethnic Populations, 2020).
Bottom line is that BMI SHOULD NOT be used as the sole indicator of how healthy someone is. Instead it should just provide more or less urgency to keep an eye on things depending on the context of the person in which that BMI number applies to.
And that is really what I want you to take away from this post. It is not about the usefulness of BMI, instead it is about how you take BMI and can or cannot apply it to you to get to a healthier spot. For some people BMI will be useless, for others it can be a useful metric that correlates nicely with other health markers. If it happens to work for you, calculating your BMI is much cheaper than virtually any other metric of health, so why not take advantage of that?
What I am really doing in this post is trying to empower you with information you can put to work for yourself in your health journey. Some pieces of information may be useful, others may not be, you need to discover what things work and don’t. If you want more information on tools and tactics you can use to improve your own health, sign up for my newsletter using the form below and I will guide you how you can apply this information to help you reach your own health goals.
References
Association of Obesity With Mortality Over 24 Years of Weight History: Findings From the Framingham Heart Study. (2018, November 16). NCBI. Retrieved September 11, 2023, from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6324399/
Correlation between epicardial adipose tissue and body mass index in New Zealand ethnic populations. (2020, June 12). PubMed. Retrieved September 13, 2023, from https://pubmed.ncbi.nlm.nih.gov/32525859/
de Carvalho, A. (2023, June 9). The paradox of obesity with normal weight; a cross-sectional study. Frontiers. Retrieved September 11, 2023, from https://www.frontiersin.org/articles/10.3389/fnut.2023.1173488/full
How useful is body mass index for comparison of body fatness across age, sex, and ethnic groups? (n.d.). PubMed. Retrieved September 13, 2023, from https://pubmed.ncbi.nlm.nih.gov/8561156/
Kannel, W. (2015, December 21). Cohort Profile: The Framingham Heart Study (FHS): overview of milestones in cardiovascular epidemiology. NCBI. Retrieved September 11, 2023, from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5156338/
Weight bias and health care utilization: a scoping review. (2019, July 22). PubMed. Retrieved September 10, 2023, from https://pubmed.ncbi.nlm.nih.gov/32800008/
This is my spin on the topic: https://carbsyndrome.com/the-truly-massive-bmi-fiasco/